Surgeon: Mark A Prissel, DPM FACFAS, Board-Certified, Fellowship Trained Foot & Ankle Surgeon
Education/training: Dr. Prissel is a fellowship trained foot and ankle surgeon and partner at The Orthopedic Foot and Ankle Center (OFAC), a practice devoted to multi-disciplinary foot and ankle care in Worthington, Ohio. In addition to his surgical practice, Dr. Prissel currently serves as co-director of the Orthopedic Foot and Ankle Center fellowship training program.
First Assistant: Vincent G. Vacketta, DPM AACFAS, Post-Graduate Fellow.
Practice: Orthopedic Foot and Ankle Center (OFAC), Worthington, OH
INTRODUCTION
Lapidus procedure is routinely used for treatment of moderate to severe Hallux Valgus (HV) deformities with 1st tarsometatarsal (TMT) joint hypermobility. Hallux Valgus is a three-dimensional deformity that has a rotational component.¹ Recent studies performed by Dayton et al. demonstrate the importance of correcting the rotational component of the deformity to achieve appropriate and complete deformity reduction.2-3 Overall, the procedure allows for powerful triplanar deformity correction resulting in a distinct change in position and rotation of the first metatarsal.
CASE PRESENTATION
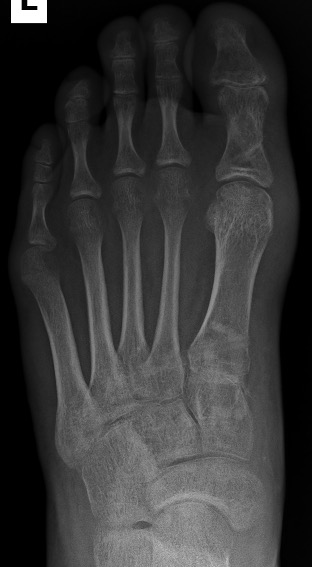
A female patient presented to our clinic with chief complaint of bilateral bunion deformity with the right foot being more symptomatic. On examination the patient exhibited HV deformity with significant medial column instability bilaterally. The first metatarsophalangeal joint range of motion was noted to be normal but with joint adaptation due to longstanding bilateral deformity. Additionally, HV interphalangeus deformity was noted bilaterally. Weight bearing (WB) radiographs demonstrated bilateral HV deformity with increased intermetatarsal, hallux valgus & hallux valgus interphalangeus angles. Conservative efforts were met with less than satisfactory results and the patient expressed interest in surgical correction though remained apprehensive to the thought of retained metallic hardware following the procedure. No other existing medical conditions were reported, besides Penicillin allergy, with no past surgical history.
WHY OSSIOfiber® IS AN IDEAL CHOICE FOR THIS PATIENT?
The patient was resistant to the use of permanent, not-absorbable fixation techniques due to concerns of potential long-term side effects of metallic hardware and possible need for subsequent removal. The OSSIOfiber® implants allow appropriate fixation stability comparable to metal, without the risk for a second surgery for hardware removal and avoiding permanent hardware retention in the body.
Preoperative Planning:
The surgical approach was determined through critical evaluation of clinical presentation, radiographic deformity, the patient’s activity and lifestyle demands, as well as her expectations.
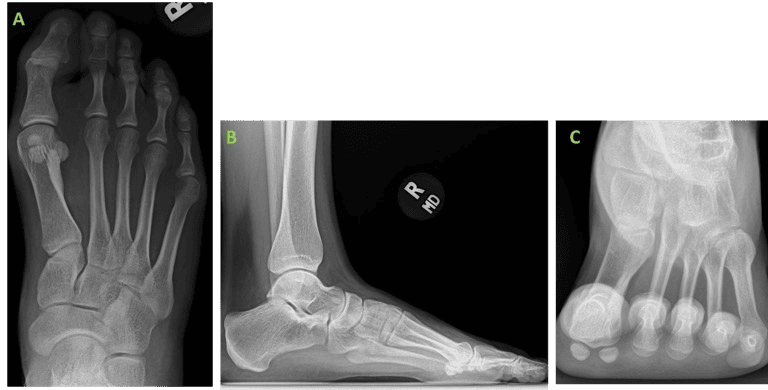
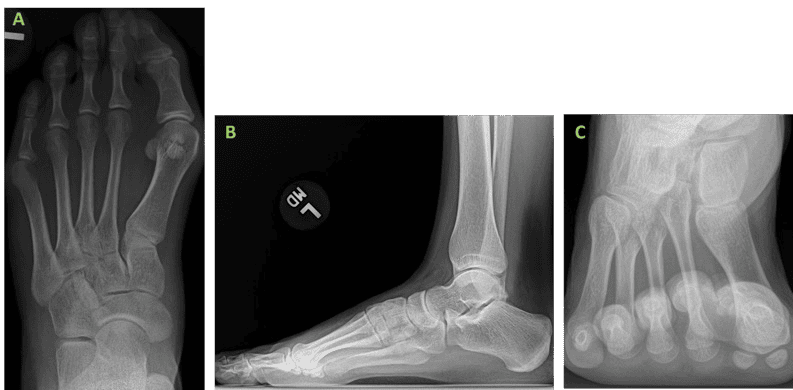
Surgical Procedure:
Patient underwent bi-lateral deformity correction 3-months apart. The surgical procedure was identical for both feet, employing the same technique using biointegrative fixation.
Procedure: Lapidus Bunionectomy.
Concomitant procedures: Calcaneal Autograft Harvest and Akin Osteotomy.
The following OSSIOfiber® fixation implants were used:
- OSSIOfiber® Compression Screw 4.0x30mm * 1 unit
- OSSIOfiber® Cannulated Trimmable Fixation Nail (CTFN) 4.0X70mm * 1 unit
- OSSIOfiber® Cannulated Trimmable Fixation Nail (CTFN) 3.0X50mm * 1 unit
- OSSIOfiber® Compression Staple 25X22mm * 1 unit
Surgical Technique Steps:
- Dissection / Access
Dorsomedial approach just medial to the extensor hallucis longus tendon. Layered dissection with careful retraction of the medial dorsal cutaneous nerve until subcapsular visualization was achieved. - Fixation site preparation:
Sharp dissection and osteotomes utilized to sever first TMT ligaments and mobilize the joint. Persistent sesamoid subluxation was observed after attempted reduction of the first metatarsal frontal plane deformity and therefore stan- dard lateral release was performed through transection of the lateral metatarso-sesamoid suspensory ligament. Lat- eral release achieved appropriate relocation of the sesamoids beneath the first metatarsal head though frontal plane rotation of first ray was still present. Next, a Hinterman pin distractor was used to expose the joint surface which was then denuded of all cartilage using osteotomes and curette. Cartilage debris was then irrigated from the fusion site. The subchondral bone plates were morselized into a healthy bleeding substrate with use of 2.5 mm drill bit and osteotome for fenestration and fish-scaling respectively. In addition, the medial aspect of the second metatarsal base was prepared in a similar fashion to allow for a “spot weld” to obviate the risk of deformity recurrence. Cancellous autograft obtained from the calcaneus via a power drill harvesting system was then delivered and packed into the first TMT fusion site. Utilizing a Steinmann pin and large reduction forceps the hallux valgus deformity was reduced in all three anatomic planes and temporary wire fixation was then placed to maintain correction after satisfactory clinical and radiographic position was achieved. - Fixation:
With the joint reduced to anatomic alignment and the fusion mass temporarily fixated, a wire associated with the 4.0mm cannulated screw was driven across the first TMT joint from dorsal-proximal to plantar-distal. Measurement for the corresponding screw was then obtained, and after appropriate drilling and tapping, the OSSIOfiber® 4.0mm compression screw was placed across the arthrodesis site in a cannulated technique. Additional compression was then afforded through use of an OSSIOfiber® compression staple. The staple drill guide was placed on the dorsal aspect of the first TMT joint just medial to the previously placed screw. After the appropriate placement of drill holes was confirmed with fluoroscopy, the compression staple was inserted on the dorsal aspect of the first TMT joint. After appropriate impaction, the staple was noted to sit flush with the dorsal cortices of the first TMT joint. Excellent compression and further stability were afforded through the supplemental staple fixation.
After fixation of the first TMT was performed, we evaluated the stability of the medial column under intra-operative fluoroscopy. There was excellent stability of the first TMT arthrodesis site though clinical and radiographic medial column instability was appreciated. In an effort to improve stability and prevent deformity reoccurrence, a guidewire for the OSSIOfiber® 4.0 cannulated nail was placed from the base of the first metatarsal to the base of the second metatarsal and from the medial cuneiform to the intermediate cuneiform in a medial to lateral direction. After confirming appropriate wire placement with fluoroscopy, appropriate measuring and drilling was performed followed by insertion of the 4.0 nail which was trimmed to the appropriate length using a sagittal saw. Special care was taken to ensure bi-cortical purchases of the second metatarsal to improve implant strength and stability. Medial column instability was then again evaluated both clinically and radiographically to confirm appropriate stability was achieved with the insertion of the OSSIOfiber® 4.0 cannulated nail.
After correction of the bunion deformity and achieving medial column stability at the TMT level, we then directed our attention to the hallux where a notable hallux interphalangeal deformity was noted. We performed dissection of the medial aspect of the proximal phalanx of the hallux in preparation for an Akin osteotomy. An oblique akin osteotomy was performed from distal-medial to proximal-lateral with care taken to maintain the lateral cortical hinge of the osteotomy. The transverse plane deformity was then reduced through the oblique osteotomy and a guidewire for the OSSIOfiber® 3.0 cannulated nail was placed from the proximal-medial base of the proximal phalanx of the hallux, across the osteotomy and exiting at the distal-lateral cortex of the proximal phalanx of the hallux. After confirming appropriate wire placement with fluoroscopy, measuring and drilling was performed followed by insertion of the 3.0 nail which was pre-trimmed to the appropriate length via sagittal saw. Upon insertion of the OSSIOfiber® 3.0 cannulated nail there was excellent stability and maintenance of correction was noted at the osteotomy site. - Closure:
Layered closure was performed using #0 and 3-0 Vicryl suture for deep tissues, and 3-0 monocryl for skin closure. A well-padded below the knee posterior splint was applied to the operated foot.
Technique Pearl:
- When using multiple OSSIOfiber® implants, we maintain the original radiopaque guidewires within the foot to allow for continued visualization of the implants throughout the operation in order to avoid inadvertent hardware convergence.
- When using OSSIOfiber® cannulated trimmable implants, we recommend trimming the implant over wire to avoid inadvertent dropping of the implant and to avoid destruction of the implant cannulation with the sagittal saw.
Post-Operative Protocol:
The use of OSSIOfiber® implants followed the same post-operative weightbearing protocols traditionally utilized for other Lapidus patients.
- Non-weight bearing: Non-weight-bearing Splint for 1 week.
- Protected weight bearing: Protected weight-bearing as tolerated in controlled ankle motion (CAM) boot at week 2, for a period of 4 weeks. Initiate physical therapy for controlled range of motion exercises.
- Full weight bearing in shoe: Transition from protected weight bearing in CAM boot into weightbearing in supportive shoe at 6 weeks with a carbon fiber plate. Continue with at- home physical therapy exercises.
Patient Follow-Up:
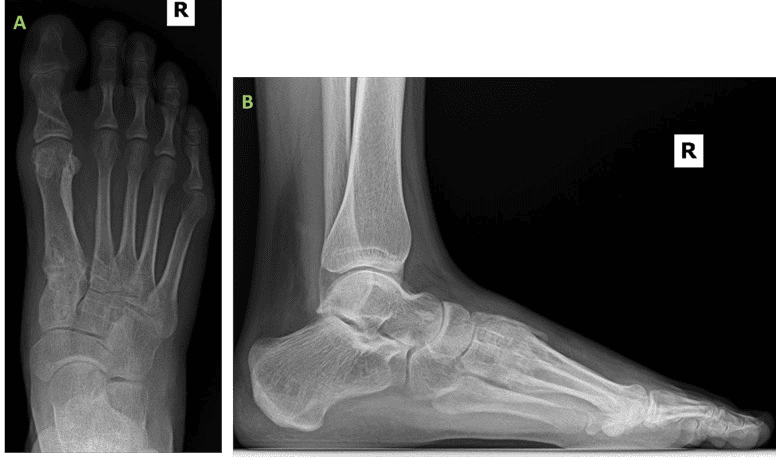
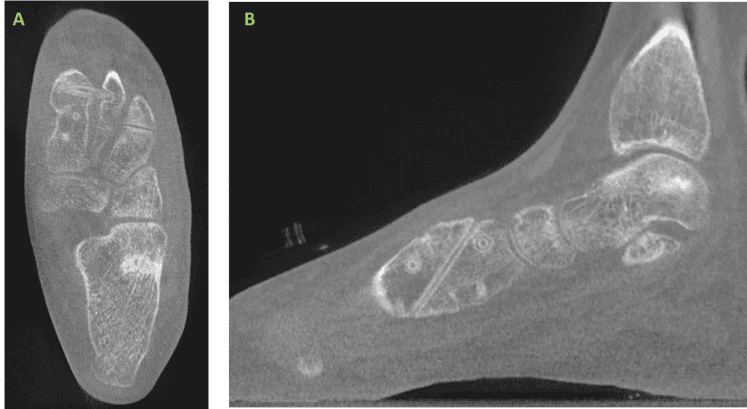
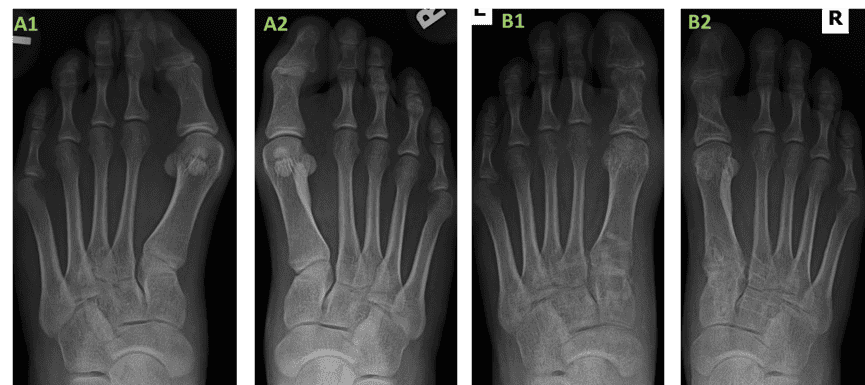
The patient underwent an unremarkable post-operative course and has proceeded to undergo an identical contralateral procedure 3-months later, employing the same technique with biointegrative fixation.
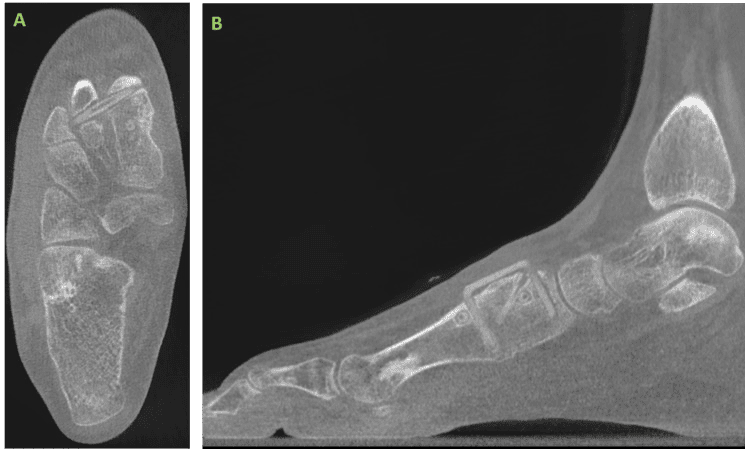
Summary:
The use of OSSIOfiber® fixation in this patient afforded successful clinical and radiographic correction of a bunion deformity without the use of retained metallic implants. The variety of OSSIOfiber® implants utilized in this case was appropriate for providing necessary osseous compression and stability to achieve osseous union and maintenance of deformity correction. Furthermore, due to the strength and stability of the OSSIOfiber® material, no deviations from early post-operative weightbearing protocols were necessary.
References
- Klemola T, Savola O, Ohtonen P, Ojala R, Leppilahti J. First Tarsometatarsal Joint Derotational Arthrodesis for Flexible Hallux Valgus: Results from Follow-Up of 3–8 Years. Scandinavian Journal of Surgery. 2017;106(4):325-331. doi:10.1177/1457496916683095
- Dayton P, Feilmeier M, Kauwe M, Hirschi J. Relationship of frontal plane rotation of first metatarsal to proximal articular set angle and hallux alignment in patients undergoing tarsometatarsal arthrodesis for hallux abducto valgus: a case series and critical review of the literature. J Foot Ankle Surg. 2013;52:348.
- Dayton P, Kauwe M, Feilmeier M. Is our current paradigm for evaluation and management of the bunion deformity flawed? A discussion of procedure philosophy relative to anatomy. J Foot Ankle Surg. 2015;54:102.
Medical professionals must use their professional judgment for patient selection and appropriate technique. Results from case studies are not predictive of results in other cases. Results may vary.
Please refer to the product instructions for use for warnings, precautions, indications, contraindications and technique. OSSIO products may not be available in all geographies. Product availability is subject to the regulatory clearances in individual markets. Please reach out to your local representative or contact OSSIO if you have questions about specific market approvals..
For more information, please visit ossio.io
® OSSIO and OSSIOfiber® are registered trademarks of OSSIO Ltd. All rights reserved 2023.
DOC-0002983 Rev 1.0
